CMA Explains
Emergency rooms are overwhelmed, millions of Canadians struggle to access primary care, surgical backlogs persist and health care workers continue to operate through intense burnout with no relief in sight.
More resources are clearly needed for the health system, including more funding. The question is who should pay, and how much?
The federal government’s 2023 budget included the most significant investment in health care in more than two decades — a $46.2-billion increase in funding to provinces and territories.
Some premiers say it’s still not enough. Health care eats up 30% to 40% of provincial and territorial budgets, and those costs are expected to increase at an average annual rate of 5.2% over the next decade — much faster than projected revenues.
Here’s how provinces and territories are currently splitting the bill for health care.
What we spend now

Canada’s total health spending was expected to reach $344 billion in 2023, or $8,740 per Canadian.

That’s about 12.1% of our GDP, making Canada a top spender among OECD countries.
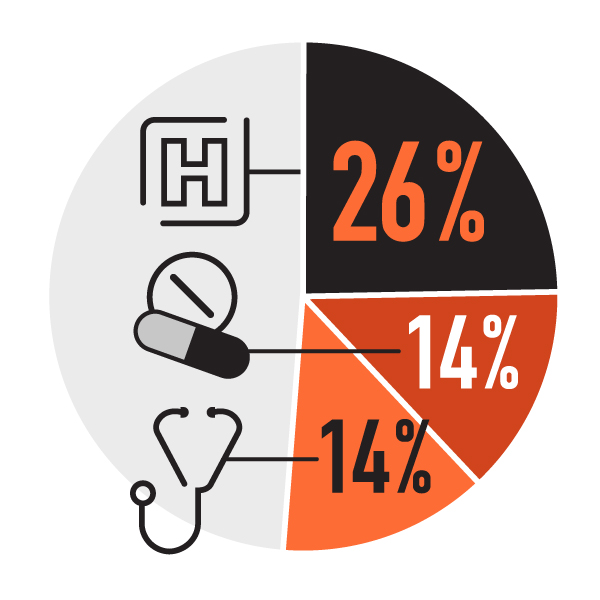
More than half of health spending goes to three areas: hospitals (26%), drugs (14%) and physicians (14%).
And, yes, equipment is expensive. One MRI machine costs $3 million.
Who pays
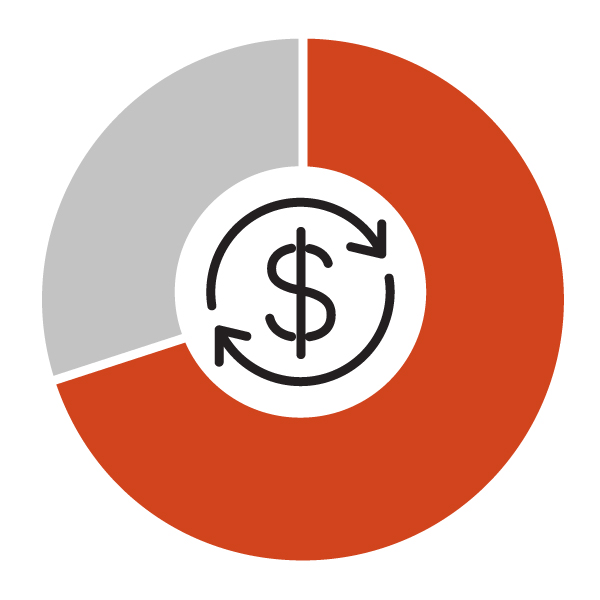
More than 70% of health care spending is publicly funded through general tax revenues.

The provinces and territories generate 78% of the cost, with the federal government providing the rest through the Canada Health Transfer (CHT).
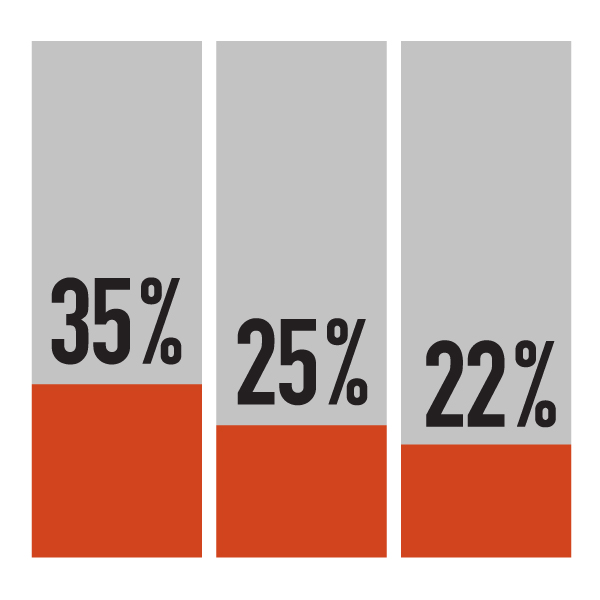
This split has been the subject of debate since Medicare was first established. At that time, the federal share was about 35%. In the late 1970s, it dropped to 25%. In 2023, the Canada Health Transfer stood at about 21.5%. The latest funding deal marked a 9.3% increase.
What does the latest health funding include?
The long-awaited health funding announced on Feb. 7, 2023 — accepted by premiers across the country — is a necessary step to transform Canada’s health care system, which requires stabilization and sustainable investment in reform. It included three core components:

An immediate and unconditional $2-billion top-up to the Canada Health Transfer (CHT) to address the pressure on emergency and operating rooms, as well as pediatric hospitals.
A 10-year federal funding commitment via the Canada Health Transfer, including a 5% annual increase for the first five years.

Bilateral agreements with each respective province or territory, a 10-year funding commitment of $25 billion.
What about provincial accountability for federal health funds?
Despite being the largest major transfer of federal funds to provinces and territories, money from the CHT does not necessarily have to be spent on health care.
In order to secure the increased CHT funding outlined in the 2023 agreement, provinces and territories must commit to:
- improving health care information collection and reporting;
- developing and using comparable performance indicators via the Canadian Institute for Health Information (CIHI); and
- adopting common standards and policies on health data.
What’s happening now?
Bilateral agreements between Ottawa and each province and territory are centered on four shared health priorities:
- expanding access to family health services, including in rural and remote areas;
- supporting health workers and reducing backlogs;
- improving access to quality mental health and substance use services; and
- modernizing the health care system with standardized health data and digital tools.
In addition, provinces and territories must commit to advancing foreign credential recognition and labour mobility for health workers, beginning with multi-jurisdictional credential recognition.
