Canada is undergoing a massive demographic shift.
There are now more Canadians over the age of 65 than under 14, and by 2036 older adults will make up a quarter of the population.
But the care we want as we grow older has not yet caught up with these changing demographics.
A recent survey by the CMA and the National Institute on Ageing found that 96% of Canadians want to age at home and live independently for as long as possible – and do everything possible to avoid going into long-term care.
This should come as no surprise: the COVID-19 pandemic exposed the severe shortcomings in the quality of care that many older adults receive in long-term care facilities. And recent data from the Canadian Institute for Health Information show that – with the proper supports in place – as many as one in ten older adults newly admitted into long-term care could have received their care at home.
Many older adults do not have access to the full spectrum of resources they need to age at home.
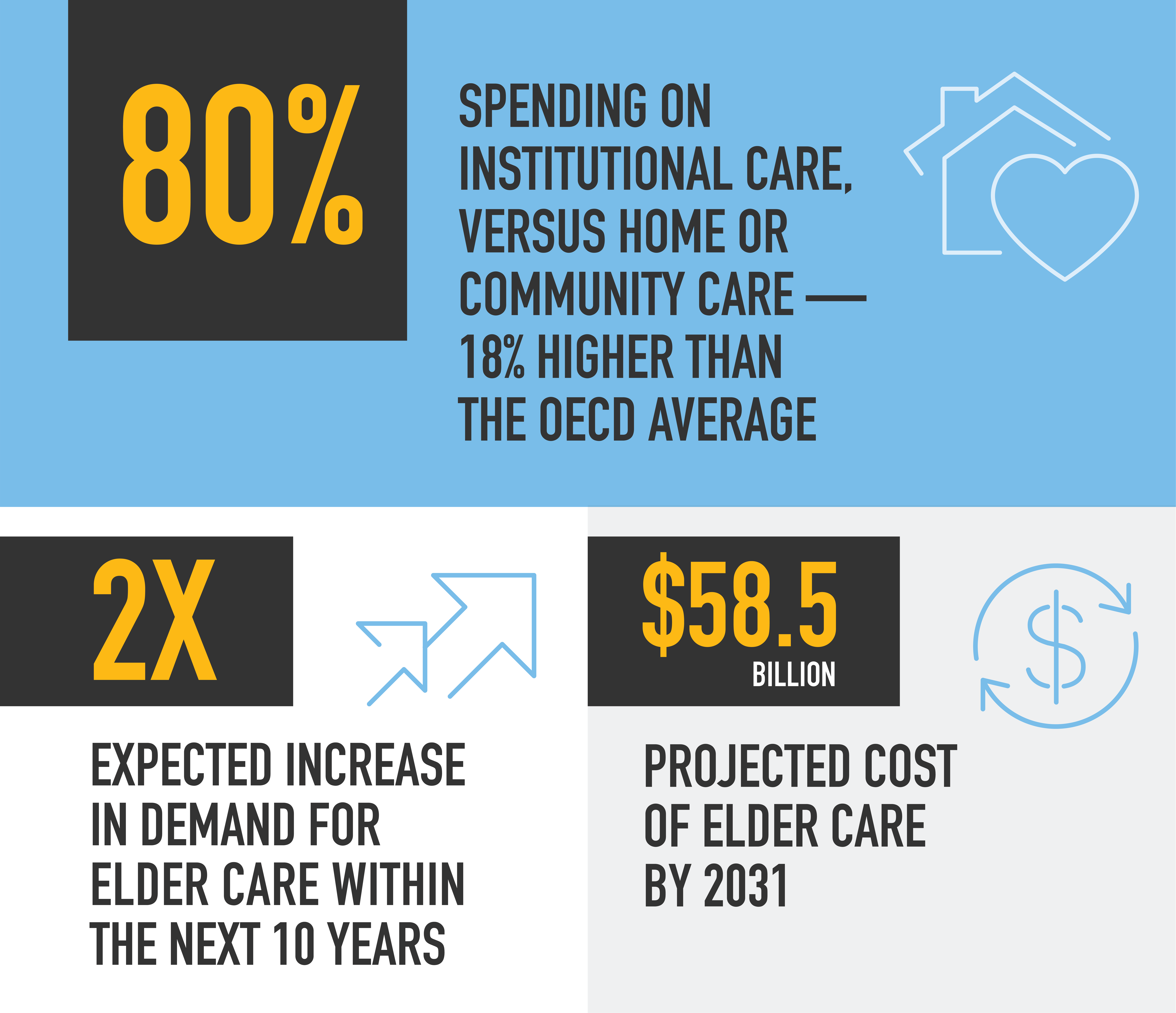
Source: Fraser Institute, Rethinking long-term care in Canada, October 2021 and Canadian Medical Association, Canada’s elder care crisis, March 2021
This leaves physicians at an impasse: They’re struggling to find the right resources and services to keep their patients at home, or to discharge them when they do need to go to the hospital.
More broadly, with no adequate level of home care and other supports in place, or desirable long-term care available to safely discharge elderly patients, hospital beds are not available for others who need them, cascading down to increasing wait times, cancelled surgeries and overcrowded emergency departments.
Fifteen percent of acute-care hospital beds in Canada are occupied by [alternate level care] patients. The CMA estimates $2.3 billion a year that could be used elsewhere in the health system if we could just break the habit of warehousing our seniors in hospitals.
— Dr. Chris Simpson, Executive Vice President, Medical, Ontario Health and former CMA president
A study commissioned by the CMA has found that demand for elder care is set to double within the next 10 years – with costs rising to $58.5 billion per year by 2031
Our advocacy for better seniors care


Along with the Canadian Nurses Association, the Canadian Society of Long-Term Care Medicine and the Canadian Social Workers Association, the CMA successfully advocated for the development of national standards for long-term care, released in 2023 by the Health Standards Organization. The goal is to ensure these standards are implemented across the country.
We also continue to call for a pan-Canadian plan to improve elder care. This includes demographics-based funding to provinces and territories to meet the needs of an aging population, which would increase the Canada Health Transfer based on each regions’ proportion of older adults and their projected health care requirements.
Our partners on aging with dignity
In collaboration with provincial and territorial medical associations, we are working to develop solutions that work for physicians across the country.
The CMA aims to collaborate with a wide range of health and non-health stakeholders, as well as elected and non-elected officials, understanding that both paid and unpaid caregivers are essential to the care older Canadians want and need, and that access to critical services is particularly challenging in rural, remote and Indigenous communities. We are committed to working in allyship with First Nations, Inuit and Métis communities, as well as people with lived experience including essential unpaid caregivers.
The CMA is also calling for a formal coalition of health and social service groups to advance solutions that will support aging with dignity at a national level.
We must do better for older adults living in Canada. The system is not only unsustainable for the next wave of older adults needing care, but also devastating to watch as individuals are presented with very few options. Ageism is real in Canada, and we can no longer turn a blind eye.
— Jean Johnston-McKitterick, CMA Patient Voice Advisory Group Member
What physicians can do to help older adults
Collaboration with physicians and learners of all ages, stages and specialties, from rural and remote communities as well as big cities, is essential for a better way forward.
